Andy
Senior Member (Voting rights)
Paywalled at https://www.cell.com/biophysj/fulltext/S0006-3495(18)31946-5Myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) is a multi-systemic illness of unknown etiology affecting millions of individuals worldwide. In this work, we tested the hypothesis that erythrocyte biophysical properties are adversely affected in ME/CFS.
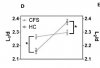
We tested erythrocyte deformability using a high-throughput microfluidic device which mimics microcapillaries. We perfused erythrocytes from ME/CFS patients and from age and sex matched healthy controls (n=14 pairs of donors) through a high-throughput microfluidic platform (5μmx5μm). We recorded cell movement at high speed (4000 fps), followed by image analysis to assess the following parameters: entry time (time required by cells to completely enter the test channels), average transit velocity (velocity of cells inside the test channels) and elongation index (ratio of the major diameter before and after deformation in the test channel). We observed that erythrocytes from ME/CFS patients had higher entry time, lower average transit velocity and lower elongation index as compared to healthy controls.
Taken together, this data shows that erythrocytes from ME/CFS patients have reduced deformability. To corroborate our findings, we measured the erythrocyte sedimentation rate for these donors which show that the erythrocytes from ME/CFS patients had lower sedimentation rates. To understand the basis for differences in deformability, we investigated changes in the fluidity of the membrane using pyrenedecanoic acid and observed that erythrocytes from ME/CFS patients have lower membrane fluidity. Zeta potential measurements showed that ME/CFS patients had lower net negative surface charge on the erythrocyte plasma membrane. Higher levels of reactive oxygen species in erythrocytes from ME/CFS patients were also observed. Using scanning electron microscopy, we also observed changes in erythrocyte morphology between ME/CFS patients and healthy controls.
Finally, preliminary studies show that erythrocytes from “recovering” ME/CFS patients do not show such differences, suggesting a connection between erythrocyte deformability and disease severity.
Edit: We have 3 threads on related or the same research by the same team:
Erythrocyte Deformability As a Potential Biomarker for Chronic Fatigue Syndrome, Davis et al (2018)
Altered Erythrocyte Biophysical Properties in Chronic Fatigue Syndrome, 2019, Saha, Davis, et al
Red blood cell deformability is diminished in patients with Chronic Fatigue Syndrome, Saha et al, 2019
Last edited by a moderator: