nataliezzz
Senior Member (Voting Rights)
The symptoms and signs of upper airway resistance syndrome: a link to the functional somatic syndromes
Avram R Gold, Francis Dipalo, Morris S Gold, Daniel O'Hearn
https://www.researchgate.net/publication/10950246_The_symptoms_and_signs_of_upper_airway_resistance_syndrome_a_link_to_the_functional_somatic_syndromes (PDF avaiable)
Study objectives: The functional somatic syndromes are associated with a variety of symptoms/signs of uncertain etiology. We determined the prevalence of several of those symptoms/signs in patients with sleep-disordered breathing and examined the relationship between the prevalence of the symptoms/signs and the severity of sleep-disordered breathing.
Design: A descriptive study without intervention.
Setting: A university sleep-disorders center located in a suburban setting.
Patients or participants: Three groups of 25 consecutively collected patients with sleep-disordered breathing. Groups varied in their apnea hypopnea indexes (AHIs) as follows: upper airway resistance syndrome (UARS) [AHI < 10/h), mild-to-moderate obstructive sleep apnea/hypopnea (OSA/H) [AHI >or= 10 to < 40/h), and moderate-to-severe OSA/H (AHI >or= 40/h).
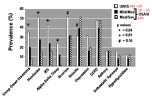
Measurements and results: Patients underwent comprehensive medical histories, physical examinations, and full-night polysomnography. The diagnosis of UARS included quantitative measurement of inspiratory airflow and inspiratory effort with demonstration of inspiratory flow limitation. The percentage of women among the patients with sleep-disordered breathing (p = 0.001) and the prevalence of sleep-onset insomnia (p = 0.04), headaches (p = 0.01), irritable bowel syndrome (p = 0.01), and alpha-delta sleep (p = 0.01) was correlated with decreasing severity of AHI group.
Conclusions: We conclude that patients with UARS, mild-to-moderate OSA/H and moderate-to-severe OSA/H differ in their presenting symptoms/signs. The symptoms/signs of UARS closely resemble those of the functional somatic syndromes.
Avram R Gold, Francis Dipalo, Morris S Gold, Daniel O'Hearn
https://www.researchgate.net/publication/10950246_The_symptoms_and_signs_of_upper_airway_resistance_syndrome_a_link_to_the_functional_somatic_syndromes (PDF avaiable)
Study objectives: The functional somatic syndromes are associated with a variety of symptoms/signs of uncertain etiology. We determined the prevalence of several of those symptoms/signs in patients with sleep-disordered breathing and examined the relationship between the prevalence of the symptoms/signs and the severity of sleep-disordered breathing.
Design: A descriptive study without intervention.
Setting: A university sleep-disorders center located in a suburban setting.
Patients or participants: Three groups of 25 consecutively collected patients with sleep-disordered breathing. Groups varied in their apnea hypopnea indexes (AHIs) as follows: upper airway resistance syndrome (UARS) [AHI < 10/h), mild-to-moderate obstructive sleep apnea/hypopnea (OSA/H) [AHI >or= 10 to < 40/h), and moderate-to-severe OSA/H (AHI >or= 40/h).
Measurements and results: Patients underwent comprehensive medical histories, physical examinations, and full-night polysomnography. The diagnosis of UARS included quantitative measurement of inspiratory airflow and inspiratory effort with demonstration of inspiratory flow limitation. The percentage of women among the patients with sleep-disordered breathing (p = 0.001) and the prevalence of sleep-onset insomnia (p = 0.04), headaches (p = 0.01), irritable bowel syndrome (p = 0.01), and alpha-delta sleep (p = 0.01) was correlated with decreasing severity of AHI group.
Conclusions: We conclude that patients with UARS, mild-to-moderate OSA/H and moderate-to-severe OSA/H differ in their presenting symptoms/signs. The symptoms/signs of UARS closely resemble those of the functional somatic syndromes.