Andy
Senior Member (Voting rights)
Post-COVID-19 syndrome (PCS) shares core clinical features with myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS), particularly persistent fatigue and post-exertional malaise (PEM). However, the prevalence of ME/CFS among PCS rehabilitation outpatients remains unclear.
Medical records of 216 PCS rehabilitation outpatients (57% female; age 47.7±12.5; January 2021 to April 2022) were retrospectively reviewed. During rehabilitation and at a six-month telephone follow-up, ME/CFS was diagnosed using the Canadian Consensus Criteria (CCC). Demographics, body mass index (BMI), FAS, and 6MWT were compared between phenotype and non-phenotype groups using logistic regression, repeated measures ANOVA, and chi-square tests (α=0.05).
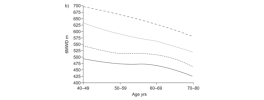
Of 216 patients, 15 (93% female; age 40.6±10.7; BMI 25.7±5.6) met ME/CFS criteria, yielding a prevalence of 6.9%. Compared with non-ME/CFS phenotype, ME/CFS phenotype patients were significantly younger (p=0.01) and predominantly female (p=0.003). Baseline FAS was significantly higher (35.8±6.4 vs. 27.8±8.6, p=0.001) and did not improve (Δ +1.3±4.5 vs. Δ -5.1±6.2, p<0.001). Baseline 6MWT was significantly lower (479±132 m vs. 540±96.1 m, p=0.02) and both groups improved over time, but between-group change was not significant (p=0.49).
Approximately 7% of PCS in outpatient rehabilitation exhibit ME/CFS, characterized by severe, persistent fatigue, female predominance, and attenuated functional gains. While the FAS is a practical screening tool, confirmation via CCC remains essential. Future studies should validate these findings and explore tailored rehabilitation strategies for patients with ME/CFS.
Open access (in German)
Medical records of 216 PCS rehabilitation outpatients (57% female; age 47.7±12.5; January 2021 to April 2022) were retrospectively reviewed. During rehabilitation and at a six-month telephone follow-up, ME/CFS was diagnosed using the Canadian Consensus Criteria (CCC). Demographics, body mass index (BMI), FAS, and 6MWT were compared between phenotype and non-phenotype groups using logistic regression, repeated measures ANOVA, and chi-square tests (α=0.05).
Of 216 patients, 15 (93% female; age 40.6±10.7; BMI 25.7±5.6) met ME/CFS criteria, yielding a prevalence of 6.9%. Compared with non-ME/CFS phenotype, ME/CFS phenotype patients were significantly younger (p=0.01) and predominantly female (p=0.003). Baseline FAS was significantly higher (35.8±6.4 vs. 27.8±8.6, p=0.001) and did not improve (Δ +1.3±4.5 vs. Δ -5.1±6.2, p<0.001). Baseline 6MWT was significantly lower (479±132 m vs. 540±96.1 m, p=0.02) and both groups improved over time, but between-group change was not significant (p=0.49).
Approximately 7% of PCS in outpatient rehabilitation exhibit ME/CFS, characterized by severe, persistent fatigue, female predominance, and attenuated functional gains. While the FAS is a practical screening tool, confirmation via CCC remains essential. Future studies should validate these findings and explore tailored rehabilitation strategies for patients with ME/CFS.
Open access (in German)