Dolphin
Senior Member (Voting Rights)
Research Article
The association between hair cortisol levels, Epstein-Barr virus infections and chronic fatigue in adolescents
Berit Elise Bergem Kongsnes,
Tarjei Tørre Asprusten
,
Vegard Bruun Bratholm Wyller
&
Maria Pedersen
Article: 2638303 | Received 20 Nov 2025, Accepted 23 Feb 2026, Published online: 02 Mar 2026
Abstract
Chronic fatigue after Epstein-Barr virus (EBV) infection is a significant health problem among adolescents, yet its underlying mechanisms remain unclear.This study investigated whether preinfection hair cortisol levels predict chronic fatigue following acute EBV infection and examined the associations between hair cortisol and concurrent fatigue during acute infection, six months postinfection, and in healthy controls.
This study is part of the CEBA project (Chronic Fatigue following Acute Epstein–Barr Virus Infection in Adolescents).
Hair samples for cortisol measurements were obtained from 192 adolescents aged 12–20 years during acute EBV infection and again six months later, and from 66 age- and sex-matched healthy controls.
Fatigue was measured by the total score on the Chalder Fatigue Questionnaire.
Group comparisons were performed using nonparametric tests, and associations were examined with linear regression analyses.
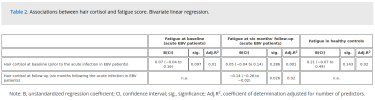
Adolescents with EBV infection had significantly higher preinfection hair cortisol levels (median 5.12, IQR: 3.27–8.76) compared with healthy controls did (median 3.90, IQR: 2.61–6.19) and with their own levels six months later (median 3.74, IQR: 2.46–6.52).
A trend toward a positive association between preinfection hair cortisol and fatigue during acute infection, became significantly negative six months later.
No associations were found among controls.
Preinfection hair cortisol concentration did not predict chronic fatigue six months after acute EBV infection.
Elevated preinfection hair cortisol may reflect stress-related vulnerability to infection, and the shifted from a positive to a negative association over time, suggests that HPA-axis alterations are more likely a consequence rather than a cause of chronic fatigue.
Keywords: