Yes, I was disappointed with this. The author is someone I know and respect, New Zealand is a small country, we see each other reasonably regularly, and yet the first I heard of the project was seeing the finished result a few days ago.
I agree with
@Ravn's summary that it is the usual mix of good bits and bad bits, and that they have focussed on the messages they wanted health professionals to hear, but have not thought enough about how it would land.
I also think there is considerable devil in the detail.
Introductory sentences
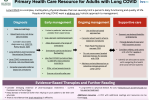
The first link there on Long COVID is to
Long COVID - a clinical update, 2024, Greenhalgh et al which has the same fundamental problem as the first sentence of this new resource. That is, it presents Long COVID as a single thing, a 'complex, multi-system disease'. This is nonsense. The definition includes people who have lost the senses of taste or smell, people who have lasting damage from being on a ventilator, people who had strokes and sepsis, people with ME/CFS, people with lung damage from the infection, myocarditis...
To roll all of those conditions and more into one thing makes efforts such as identifying risk factors or suggesting management and treatments completely meaningless.
The Greenhalgh paper also has a number of other problems, including advocating for the usual range of 'holistic' multidisciplinary rehabilitation approaches that have no proven efficacy and waste people's time and energy. It sends mixed messages about exercise, suggesting that rehabilitation therapies work well for some people. Figure 3 in particular is a travesty of misinformation. The paper does not acknowledge that a considerable proportion of people with Long COVID have ME/CFS.
The Greenhalgh paper was not a good one to link to. It's also not great to give Greenhalgh or another author, Sivan, any more profile than can be helped - they and their ideas have not been helpful to people with ME/CFS.
Getting back to the introductory sentences of this resource:
The first sentence describes Long COVID as a 'complex .. disease'. We've talked about that word 'complex' a lot on the forum. Advocates trying to convey something about how awful the disease is end up shooting themselves and us in the foot. Many health professionals hear 'complex' and think 'at least partly psychological' - it's almost a code word for that. And, what is it really adding there? If the authors are trying to say that Long COVID has a heterogeneous presentation, then they should say that. If they are trying to say that it is poorly understood, then they should say that.
'Multisystem' has similar problems. We don't have any great evidence that any particular system is being affected. Most diseases are multisystem in a limited sense - the body is one thing and if there is an infection for example, there will be symptoms in many parts of it. Using 'multisystem' there in an attempt to explain that people have lots of symptoms actually just misleads people about the evidence (i.e. the lack of evidence).
The second introductory sentence says 'People with long COVID want a whānau ora, holistic approach to management'. 'Whānau ora' links through to a graphic about what Long Covid services should be -
here. Whānau ora literally means 'healthy families'. A lot of this is good:
- Culturally safe
- Addresses systemic violence
- Provide practical support
- Protection from the financial burden of being unwell
- Services to support those who care for us
- Grief counselling
But, I would have liked to talk to the people who informed and created this work about the risks of siloing off Long Covid services, and for calling for holistic 'integrated' services. Surely we want every person with a disabling chronic illness to have help with those points above? And, the big risk with calling for services that
'integrate traditional and alternative healing practices with conventional medicine',
with calling for alternative therapies specifically for Long Covid, is that it makes the illness appear very 'fringe'.
We've discussed these problems on the thread about what we would like ME/CFS and LC services to look like. 'Holistic and integrated' sounds really nice, but many health professionals read that as 'we can make people happy and well by offering them a mindfulness course'. We actually need people and doctors too feeling a bit motivated about the fact that there is no useful evidence based treatment. We don't need people fobbed off into a quiet corner with healing crystals, acupuncture and a course on how to breathe better, trialling their next expensive supplement because they have been assured 'it works for some people'.
It is not at all accurate to say that 'people with Long COVID' want such an approach that integrates alternative therapies. Not everyone does. Perhaps as Ravn noted, the process of creating this resource selected for the people who are more likely to think certain things.
I think if the consequences of promoting this integration of alternative therapies were explained, including the massive risk of exacerbating inequities, encouraging people to not think scientifically and confirming the view many doctors hold of Long COVID and ME/CFS as psychosomatic conditions, some of the people who signed on to this approach might change their mind.
At a time when we desperately need to be educating people with LC and ME/CFS not to waste their money on unevidenced supplements and therapies and to become more critical of people offering cures, we have this resource being sent out to all GPs in New Zealand, advocating for alternative therapy integration.