Migraine prevalence by age and sex in the United States: A life-span study
Abstract
The present study assessed age- and sex-specific patterns of migraine prevalence in a US population of 40,892 men, women, and children who participated in the 2003 National Health Interview Survey. Gaussian mixture models characterised the relationship between migraine, age, and sex.
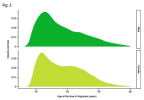
Migraine prevalence was 8.6% (males), 17.5% (females), and 13.2% (overall) and showed a bimodal distribution in both sexes (peaking in the late teens and 20s and around 50 years of age). Rate of change in migraine prevalence for both sexes increased the fastest from age 3 years to the mid-20s.
Beyond the age of 10 years, females had a higher prevalence of migraine than males. The prevalence ratio for females versus males was highest during the female reproductive/child-bearing years, consistent with a relationship between menstruation and migraine. After age 42 years, the prevalence ratio was approximately 2-fold higher in women.
Web | DOI | PDF | Cephalalgia | Open Access
Victor, TW; Hu, X; Campbell, JC; Buse, DC; Lipton, RB
Abstract
The present study assessed age- and sex-specific patterns of migraine prevalence in a US population of 40,892 men, women, and children who participated in the 2003 National Health Interview Survey. Gaussian mixture models characterised the relationship between migraine, age, and sex.
Migraine prevalence was 8.6% (males), 17.5% (females), and 13.2% (overall) and showed a bimodal distribution in both sexes (peaking in the late teens and 20s and around 50 years of age). Rate of change in migraine prevalence for both sexes increased the fastest from age 3 years to the mid-20s.
Beyond the age of 10 years, females had a higher prevalence of migraine than males. The prevalence ratio for females versus males was highest during the female reproductive/child-bearing years, consistent with a relationship between menstruation and migraine. After age 42 years, the prevalence ratio was approximately 2-fold higher in women.
Web | DOI | PDF | Cephalalgia | Open Access