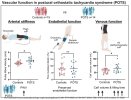
Central arterial stiffness, flow-mediated dilation and venous function in postural orthostatic tachycardia syndrome POTS
Postural Orthostatic Tachycardia Syndrome (POTS) is a debilitating disorder characterised by excessive increases in heart rate upon standing and poor orthostatic tolerance. Impairments in large artery, endothelial, and venous function may collectively, or individually, result in excessive blood pooling and impaired venous return, or other inadequate vascular response to standing, thus contribute to POTS.
Herein, we tested the hypothesis that patients with POTS would exhibit reduced large artery stiffness, enhanced endothelial function, and greater lower limb venous pooling while standing, compared to healthy controls.
Fourteen participants with a clinical diagnosis of POTS and 15 age matched controls (all females; median age [IQR]; 21 [19-37] years, p=0.769) were recruited. Central arterial stiffness was determined using carotid-femoral pulse wave velocity (cfPWV; SphygmoCor). Endothelial function was assessed using brachial artery flow-mediated dilation (FMD) following a 5-minute forearm occlusion at 200 mmHg. Functional measures of calf venous volume and filling time (90% maximal venous filling) were acquired (air plethysmography) whilst standing.
cfPWV was increased in people with POTS ([Mean±SD] 5.5±0.9 vs. 4.8±0.4, p=0.031) while FMD was not different between groups (p=0.854). During standing, calf venous volume was 29% greater in people with POTS (p=0.048) and venous filling time was almost twice as long (404±199 vs. 207±99 s; p=0.003).
These findings indicate that people with POTS exhibit increased central arterial stiffness, preserved endothelial function, and increased calf venous filling during standing. Such differences in lower limb venous filling dynamics on standing likely contribute to the orthostatic intolerance that characterises POTS.
Web | DOI | PDF | American Journal of Physiology-Heart and Circulatory Physiology | Open Access
Greer E Pugh; Kate N Thomas; Jui-Lin Fan; James P Fisher
Postural Orthostatic Tachycardia Syndrome (POTS) is a debilitating disorder characterised by excessive increases in heart rate upon standing and poor orthostatic tolerance. Impairments in large artery, endothelial, and venous function may collectively, or individually, result in excessive blood pooling and impaired venous return, or other inadequate vascular response to standing, thus contribute to POTS.
Herein, we tested the hypothesis that patients with POTS would exhibit reduced large artery stiffness, enhanced endothelial function, and greater lower limb venous pooling while standing, compared to healthy controls.
Fourteen participants with a clinical diagnosis of POTS and 15 age matched controls (all females; median age [IQR]; 21 [19-37] years, p=0.769) were recruited. Central arterial stiffness was determined using carotid-femoral pulse wave velocity (cfPWV; SphygmoCor). Endothelial function was assessed using brachial artery flow-mediated dilation (FMD) following a 5-minute forearm occlusion at 200 mmHg. Functional measures of calf venous volume and filling time (90% maximal venous filling) were acquired (air plethysmography) whilst standing.
cfPWV was increased in people with POTS ([Mean±SD] 5.5±0.9 vs. 4.8±0.4, p=0.031) while FMD was not different between groups (p=0.854). During standing, calf venous volume was 29% greater in people with POTS (p=0.048) and venous filling time was almost twice as long (404±199 vs. 207±99 s; p=0.003).
These findings indicate that people with POTS exhibit increased central arterial stiffness, preserved endothelial function, and increased calf venous filling during standing. Such differences in lower limb venous filling dynamics on standing likely contribute to the orthostatic intolerance that characterises POTS.
Web | DOI | PDF | American Journal of Physiology-Heart and Circulatory Physiology | Open Access