Maybe, in addition, but pain and malaise and other sickness symptoms are more than enough to explain this behaviour. For sure I have no other reason, and I've never really come across anyone saying different as far as their own experience goes.We actually don’t know the causal pathways here. I think it’s reasonable that the pain and malaise might cause some changes in behaviour, but I wouldn’t be surprised if disease can cause changes in behaviour directly as well.
You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
Brain Endothelial- and Epithelial-Specific Interferon Receptor Chain 1 Drives Virus-Induced Sickness Behavior and Cognitive Impairment, 2016, Blank +
- Thread starter Hutan
- Start date
Utsikt
Senior Member (Voting Rights)
We probably wouldn’t be able to differentiate between them so that’s no surprise.I've never really come across anyone saying different as far as their own experience goes.
jnmaciuch
Senior Member (Voting Rights)
The paper shows no pDCs infiltration in the skin as well in cases of cutaneous lupus. But yes you’re right that things might be slightly different in different microenvironments, or if the stimulation is only sporadic during PEM.I haven't looked closely at that paper, I've got a headache and am struggling - but isn't that Nature paper looking at pDCs in peripheral blood only? They might be quite different when in lymph tissue or elsewhere?
We might only need the pDCs to be doing an interferon thing in PEM. So, not necessarily prolonged activation. Obviously lupus isn't ME/CFS, so things can be different.
There was a very small study somewhere that was suggesting that IRF7 is upregulated in ME/CFS - and IRF7 is part of the pDC mechanism.
I was thinking along similar lines hypothesizing that TLR9 stimulation from mtDNA during muscle use or repeated neuron firing could contribute to PEM, though that would likely be involving tissue resident macrophages rather than circulating cells. The trick would be figuring out what TLR stimulus is really only present during the trigger for PEM (or at least in much higher amounts), which is what lead me to think of mtDNA.
[Edit: and, of course, thinking what other mechanism would be constantly misbehaving to produce baseline symptoms outside of PEM.]
Last edited:
V.R.T.
Senior Member (Voting Rights)
How goes your quest for muscle samples?The paper shows no pDCs infiltration in the skin as well in cases of cutaneous lupus. But yes you’re right that things might be slightly different in different microenvironments, or if the stimulation is only sporadic during PEM.
I was thinking along similar lines hypothesizing that TLR9 stimulation from mtDNA during muscle use or repeated neuron firing could contribute to PEM, though that would likely be involving tissue resident macrophages rather than circulating cells. The trick would be figuring out what TLR stimulus is really only present during the trigger for PEM (or at least in much higher amounts), which is what lead me to think of mtDNA.
[Edit: and, of course, thinking what other mechanism would be constantly misbehaving to produce baseline symptoms outside of PEM.]
Appreciate you may not be able to divulge everything but curious to know how your work is progressing.
jnmaciuch
Senior Member (Voting Rights)
Slow, unfortunately, but will soon be sending out some more collaboration requests. My mentors fully support me pursuing this as a passion project but I’m obligated to prioritize the projects that are funding my PhD and my program’s academic requirements first. Which sadly has left very little time and energy left over, as I’m sure folks here can intuit.How goes your quest for muscle samples?
Appreciate you may not be able to divulge everything but curious to know how your work is progressing.
Last edited:
V.R.T.
Senior Member (Voting Rights)
Totally understandable! I remember trying to do academia with ME, it was hard going.Slow, unfortunately, but will soon be sending out some more collaboration requests. My mentors fully support me pursuing this as a passion project but I’m obligated to prioritize the projects that are funding my PhD and my program’s academic requirements first. Which sadly has left very little time and energy left over, as I’m sure folks here can intuit.
Hope the collaboration requests are fruitful!
hotblack
Senior Member (Voting Rights)
If plasmacytoid dendritic cells are involved and their characteristic is that they produce very large quantities of type I interferon (wikipedia says up to 1,000 times more than other cell types, mainly IFN-α and IFN-β), why do we not see very large quantities of interferon in people with ME/CFS? Even if only in PEM, we would surely have seen such elevated levels crop up somewhere wouldn’t we?
jnmaciuch
Senior Member (Voting Rights)
pDCs were found to be the main source during actual infection because they are specialized to produce those high levels of IFN in response to activation of receptors for detecting pathogenic particles. But pDCs aren’t the only source of type I interferon. If interferon in ME/CFS was being produced by neurons themselves, which they have the capability to do, you would probably not see it in the blood stream at all unless the BBB is compromised. It’s also theoretically possible that there’s no interferon and the CXCL10 from brain epithelial cells (that is directly responsible for sickness behavior) is triggered by something else.If plasmacytoid dendritic cells are involved and their characteristic is that they produce very large quantities of type I interferon (wikipedia says up to 1,000 times more than other cell types, mainly IFN-α and IFN-β), why do we not see very large quantities of interferon in people with ME/CFS? Even if only in PEM, we would surely have seen such elevated levels crop up somewhere wouldn’t we?
If interferon does reach detectable levels in the blood only during PEM from another tissue source like muscles, I don’t know of any existing study that would have been able to detect it. The few studies we have performed screens on day 2 of CPET, so it’s unclear whether the participants were actually in PEM. Even if they were, interferons are orders of magnitude less abundant than other metabolites (even when pumped out by pDCs) and fall below detection limits in unbiased screening methods. You would have to set up an experiment to deliberately measure interferon. I only know of Rob Phair doing this measurement, but it was not during PEM.
jnmaciuch
Senior Member (Voting Rights)
Another offhand thought: CXCR3 (the receptor for CXCL10) is widely expressed on neurons. This is in contrast to the prostaglandin receptor on a specific type of neuron which was found to mediate warmth seeking and loss of appetite (but not lethargy) during infection in this paper:
It’s an interesting difference to note because CXCR3 activation seems to modulate neuron activity, rather than acting as a stimulus that generates an action potential. For example, this paper found that chronic CXCL10 signaling altered GABA/glutamate signaling, inducing hyperexcitability of neurons (side note, this seems very much in line with sensory sensitivity and the beneficial effect of medications like Xanax that members report).
So it suggests that unlike warmth seeking/loss of appetite/fever, the lethargy and malaise parts of sickness behavior are better explained by a global modulation of neuron function across many brain regions rather than the activation of specific neural circuits.
A preoptic neuronal population controls fever and appetite during sickness
Osterhout, Kapoor, Eichhorn, Vaughn, Moore, Ding Liu, Lee, DeNardo, Liqun Luo, Xiaowei Zhuan, Dulac
Abstract
During infection, animals exhibit adaptive changes in physiology and behaviour aimed at increasing survival. Although many causes of infection exist, they trigger similar stereotyped symptoms such as fever, warmth-seeking, loss of appetite and fatigue1,2. Yet exactly how the nervous system alters body temperature and triggers sickness behaviours to coordinate responses to infection...
Osterhout, Kapoor, Eichhorn, Vaughn, Moore, Ding Liu, Lee, DeNardo, Liqun Luo, Xiaowei Zhuan, Dulac
Abstract
During infection, animals exhibit adaptive changes in physiology and behaviour aimed at increasing survival. Although many causes of infection exist, they trigger similar stereotyped symptoms such as fever, warmth-seeking, loss of appetite and fatigue1,2. Yet exactly how the nervous system alters body temperature and triggers sickness behaviours to coordinate responses to infection...
- CRG
- fever hypothalamus neurological sickness behaviour
- Replies: 16
- Forum: Other health news and research
It’s an interesting difference to note because CXCR3 activation seems to modulate neuron activity, rather than acting as a stimulus that generates an action potential. For example, this paper found that chronic CXCL10 signaling altered GABA/glutamate signaling, inducing hyperexcitability of neurons (side note, this seems very much in line with sensory sensitivity and the beneficial effect of medications like Xanax that members report).
So it suggests that unlike warmth seeking/loss of appetite/fever, the lethargy and malaise parts of sickness behavior are better explained by a global modulation of neuron function across many brain regions rather than the activation of specific neural circuits.
hotblack
Senior Member (Voting Rights)
Thanks @jnmaciuch I’m very much into the more general interferon theories now, I was just unsure of how pDCs fit in, as such a large signal seems like something we would have noticed even if only in some patients in some studies. But if it’s that difficult to measure perhaps not!
Great to see mention of the triggering around neurons too. This was something I was thinking about. So as well as having the say, physical activity trigger at muscle cells discussed before, you could also have these entirely localised nerve cell triggers?
Could there be the same underlying mechanism but some timing differences between physical and cognitive PEM explained here too (if present, maybe this is a good question for people)?
I’m picturing some localised cognitive or sensory load triggering the mitochondria/interferon thing which quickly reaches say endothelial cells and astrocytes. While perhaps the physical PEM needing interferon to reach a certain threshold and spillover and get around the body?
Great to see mention of the triggering around neurons too. This was something I was thinking about. So as well as having the say, physical activity trigger at muscle cells discussed before, you could also have these entirely localised nerve cell triggers?
Could there be the same underlying mechanism but some timing differences between physical and cognitive PEM explained here too (if present, maybe this is a good question for people)?
I’m picturing some localised cognitive or sensory load triggering the mitochondria/interferon thing which quickly reaches say endothelial cells and astrocytes. While perhaps the physical PEM needing interferon to reach a certain threshold and spillover and get around the body?
jnmaciuch
Senior Member (Voting Rights)
That’s the thought, at least. If the feedback loop is dependent on calcium flux then it could theoretically occur anywhere that happens—skeletal muscle, neurons, etc. I was thinking that in more severe cases, even the constant smooth muscle contractions in the heart and intestines could potentially contribute to this disease mechanism.So as well as having the say, physical activity trigger at muscle cells discussed before, you could also have these entirely localised nerve cell triggers?
Those are both great questions! I don’t think enough is known about these mechanisms to say for sure, especially since I’m taking some leaps from all these findings for the sake of pulling together a hypothesis. But the line of thinking definitely makes sense and would be interesting to get some more data on.Could there be the same underlying mechanism but some timing differences between physical and cognitive PEM explained here too (if present, maybe this is a good question for people)?
I’m picturing some localised cognitive or sensory load triggering the mitochondria/interferon thing which quickly reaches say endothelial cells and astrocytes. While perhaps the physical PEM needing interferon to reach a certain threshold and spillover and get around the body?
Another potential hitch in the theory is finding out whether the interferon receptor is expressed on both sides of the BBB. If it’s only expressed on the side that would be exposed to circulating cells, then you’d have to explain how interferon from neurons on the other side of the barrier could lead to PEM—perhaps through increased BBB permeability in people that are more severe. Not everyone gets PEM from cognitive activity so some additional piece like this might be necessary to explain that.
jnmaciuch
Senior Member (Voting Rights)
ME/CFS Science Blog's new article linked to a review of cytokine assays done in CSF
There were 4 studies, and CXCL10 was measured in 2 of them. If CXCL10 drives feelings of malaise in ME/CFS, you might expect it to be higher in the CSF compared to healthy controls.
One study (Hornig et al.) found elevated levels (n=32 ME/CFS, 19 controls):
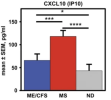
I don't think these p-values were corrected. I'll note that the very high level in MS biobank samples could either be due to active immune processes in the brain, or the fact that synthetic interferon is a standard treatment for MS (and CXCL10 is a strongly induced interferon-stimulated gene). The 19 controls were also from a biobank--the samples were only included if there was no sign of infection in the CNS, but they are not truly healthy controls since the samples were taken to try to diagnose an unknown health issue.
In contrast, Peterson et al. (n=18 ME/CFS, 5 controls) reported only one significantly different finding, and it was IL-10 not CXCL10. Interestingly 2/4 studies found decreased IL-10 in ME/CFS, which is a cytokine that counteracts STAT1-dependent interferon-stimulated gene signaling. But a third study found it was elevated, so seems inconsistent. IL-10 is also involved in and induced by other signaling so it would be considered a poor proxy for the possible influence of IFN/CXCL10.
Unfortunately I am not sure if there's a good way to follow up on this. The next logical question would be whether CXCL10 is most elevated when participants are in active PEM (or if it is significantly higher the most severe someone is). But in either case, I don't think it would be particularly ethical to subject someone in active PEM or a severe pwME to an LP
In this article, we have made a comprehensive overview of research findings on the immune system in patients with myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS). In contrast to what is frequently claimed, current data do not suggest that (low-grade) inflammation is a key driver of ME/CFS symptoms. There have been major studies into viral persistence, antibodies, and cytokines, but with mostly null results. The most consistent findings in the ME/CFS literature on the immune system over the past 40 years are reduced natural killer cell cytotoxicity and increased levels of...
- ME/CFS Science Blog
- autoantibodies immune system me/cfs science blog nk cells viral persistence
- Replies: 75
- Forum: ME/CFS research
There were 4 studies, and CXCL10 was measured in 2 of them. If CXCL10 drives feelings of malaise in ME/CFS, you might expect it to be higher in the CSF compared to healthy controls.
One study (Hornig et al.) found elevated levels (n=32 ME/CFS, 19 controls):

I don't think these p-values were corrected. I'll note that the very high level in MS biobank samples could either be due to active immune processes in the brain, or the fact that synthetic interferon is a standard treatment for MS (and CXCL10 is a strongly induced interferon-stimulated gene). The 19 controls were also from a biobank--the samples were only included if there was no sign of infection in the CNS, but they are not truly healthy controls since the samples were taken to try to diagnose an unknown health issue.
In contrast, Peterson et al. (n=18 ME/CFS, 5 controls) reported only one significantly different finding, and it was IL-10 not CXCL10. Interestingly 2/4 studies found decreased IL-10 in ME/CFS, which is a cytokine that counteracts STAT1-dependent interferon-stimulated gene signaling. But a third study found it was elevated, so seems inconsistent. IL-10 is also involved in and induced by other signaling so it would be considered a poor proxy for the possible influence of IFN/CXCL10.
Unfortunately I am not sure if there's a good way to follow up on this. The next logical question would be whether CXCL10 is most elevated when participants are in active PEM (or if it is significantly higher the most severe someone is). But in either case, I don't think it would be particularly ethical to subject someone in active PEM or a severe pwME to an LP
Last edited:
