A nationwide healthcare program for functional somatic disorders (FSD) in Denmark
You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
Opinion A nationwide healthcare program for functional somatic disorders (FSD) in Denmark, 2026, Gormsen et al
- Thread starter rvallee
- Start date
More fantasy from Per Fink and his colleagues. Hard to classify, the article is published as a "short communication", so it's not research by even the (very low) standards of the Journal of psychosomatic medicine, and there isn't really a better option than opinion. It's not a review either, just a commentary. It's pretty much fiction, but there is no fiction category so whatever.
This could have been written for astrological or homeopathic medicine dealing with, uh, cosmic micro-injuries, as a different model for discriminated chronic illnesses and not much would be different.
What's fascinating about this is that it's basically self-yesmanning, people who simply delude themselves that they're always right using their own opinion as a guide, writing down their own opinion as fact, then citing as evidence that they are correct, mostly by simply having done the thing with no consideration for efficacy. Weird stuff.
This could have been written for astrological or homeopathic medicine dealing with, uh, cosmic micro-injuries, as a different model for discriminated chronic illnesses and not much would be different.
What's fascinating about this is that it's basically self-yesmanning, people who simply delude themselves that they're always right using their own opinion as a guide, writing down their own opinion as fact, then citing as evidence that they are correct, mostly by simply having done the thing with no consideration for efficacy. Weird stuff.
Jonathan Edwards
Senior Member (Voting Rights)
Bizarre to lay out an abstract as if it is a scientific study when all it is is describing what was done according to certain beliefs.
ME/CFS is clearly included in the concept of Functional Somatic Syndromes, and Long COVID.Over the past decades, numerous specialty-specific functional somatic syndromes (FSS) such as irritable bowel syndrome, fibromyalgia, chronic fatigue syndrome, and most recently long-COVID have been introduced, and new syndromes continue to emerge. Studies consistently demonstrate a huge overlap between these syndromes [9,10]. The unifying evidence-based diagnosis bodily distress syndrome (BDS) was introduced in 2007 [2] This diagnosis has been rigorously validated across clinical settings [3], and it has been shown to be able to replace the functional syndrome diagnoses [9, 24]. In 2019, the BDS diagnosis was included in the Danish ICD-10 as a neutral R-diagnosis, thus avoiding controversies about psychiatric versus non-psychiatric classification [1,11]. The terminology was, however, changed to FSD to avoid confusion with the new but different ICD-11 diagnosis termed bodily distress disorder [1].
It's a bit weird to conflate people reporting symptoms after a vaccine with functional syndromes. Of course the linking of symptoms with a vaccine could well be wrong, but, in an environment where there is a lot of promotion of the idea of vaccine injury following a specific vaccine, it's to be expected. It doesn't mean the symptoms being reported are not true, it's just the linkage with the vaccine that becomes suspect.In response, the Danish Health Authority in 2018 initiated a national strategy to establish FSD as an acknowledged medical field . Several factors contributed to the development of a national strategy for FSD at that time. First, a convergence of key individuals with a strong interest in FSD emerged, including Professor Per Fink and the Health Authority Director General Søren Brostroem. In addition, a vaccination crisis arose when public criticism intensified following reports of multiple symptoms in young women attributed to the new HPV vaccine. This turning point led to several initiatives with the new national strategy as point of departure: the development of more specialized services, national public information, pre and post clinical education of healthcare professionals, a quality database aiming to improve care and reduce stigma and the establishment of the Danish Society for Functional Disorders.
That's a cunning plan. GPs are the gatekeepers to specialist and hospital care, so they are the ones that need to be trained to label anything not particularly clear as FSD, thereby ensuring that people with that label are quickly directed away from expensive investigations.The Danish healthcare system is tax-funded, and 98% of all Danes are listed with general practices, where general practitioners (GPs) serve as gatekeepers to specialist and hospital care. As part of the national FSD strategy from 2018, the Danish Health Authority mandated the development of FSD recommendations across all levels of care, i.e., local, regional, and highly specialized—ensuring equal access to coordinated and evidence-based care nationwide. The program is based on a stepped-care model where a minimum of 95% of patients are expected to be treated in primary care and at a non-specialized hospital care level. The recommendations encompass a diagnosis of FSD,specialized clinical services, and a clinical toolkit for GPs. Furthermore, physicians in relevant medical specialties are required to be skilled in the diagnosis and basic management of FSD (see Table 1).
I find all the rationale for the various labels (e.g. BDD, BDS, FSD) rather unclear and am not much motivated to understand it. But, the end result seems to be that, even if your GP has previously assessed you to be a person with no mental health issues, that is no protection from an FSD diagnosis.FSD unified the previous diagnoses of functional syndromes and is a central feature of the Danish model. Another rationale for developing the diagnosis FSD, was that the ICD-10/DSM-IV diagnosis somatoform disorder required symptoms to be attributed to a mental origin, which in
many cases could not be established.
Outpatient treatment clinics
Inpatient services
At the same time, a systematic training program for general practice trainees was developed, alongside the establishment of a course in FSD at the Medical School. Since 2019, the five clinics have provided evidence-based, multimodal treatment delivered by a multidisciplinary staff including physicians, psychologists, physiotherapists, psychomotor therapists, nurses, and social workers while also functioning as hubs for professional training. The treatment programs have over the years been adjusted in accordance with the latest research to ensure a high standard of care.
A bio-psycho-social illness model and treatment options for FSD are presented. Treatment may include patient education, graded exercise therapy (GET), pharmacotherapy, and psychotherapy including group, individual and internet based
Inpatient services
Two highly specialized inpatient units were established as a collaboration between the neurological rehabilitation and the FSD departments in the Capital Region and the Central Denmark Region. They provide care for patients with severe FSD including those with complex functional neurological disorders and CFS/ME who often have very low functional levels and may be bedbound and therefore cannot be managed in the outpatient service.
Pre-admission involves triage, diagnostic assessment and motivation
Diagnostic assessment and motivational work follow outpatient clinic procedures.
Inpatient admission at HHN consists of three phases: an initial assessment phase (1–2 weeks) to establish a therapeutic alliance; a specific rehabilitation phase with individualized treatment plans including graded physical exercise, environmental therapy, psychoeducation, psychotherapy, and home rehabilitation; and a discharge phase focused on municipal transition, coordinated post-discharge care, and follow-up. Aftercare continues at the Department of Functional Disorder’s outpatient clinic, AUH.
TerrifyingA nationwide healthcare program for functional somatic disorders (FSD) in Denmark
Background
Functional Somatic Disorders (FSD) are prevalent, costly for society and cause significant suffering for patients. The healthcare system has previously failed to provide adequate care for these patients, leading to prolonged and fragmented diagnostic processes. Major obstacles have been the lack of a clear classification of FSD and lack of prioritization of diagnosis and treatment of FSD by other medical specialties.
Methods
In 2018, the Danish Health Authority issued national recommendations to improve the quality of care for FSD nationwide across all levels of the healthcare system. The recommendations provide a framework to ensure evidence-based care.
Results
As part of the Danish program, FSD is included in the Danish medical specialty planning. The first Danish specialist department for FSD was established in 1999, followed by an additional four departments in 2019. Furthermore, two highly specialized inpatient services have been established. The unified FSD diagnosis is included in the Danish ICD-10 under the “neutral” and nonspecific R chapter. A national clinical database “FuncData” has been established as well as a compulsory educational program for GPs in training for specialization.
Conclusion
The Danish national strategy for FSD has been successfully implemented and integrated into the Danish health care system, achieving organizational integration and high levels of patient and physician satisfaction. The program provides a comprehensive, accessible, and evidence-based framework for managing FSD through a stepped-care approach and may serve as an inspiration for implementation in other countries.
Sounds like a manifesto for forcing a dystopia where huge amounts of patients with real illnesses get systemically destroyed /taken apart /removed from rights
When I think of where the evidence is on what they’ve been up to and how the papers etc not being retracted is just due to the same small groups / number of individuals being those writing the same reviews , circumventing consent by not declaring conflicts of interests financial interests etc
Vs the now huge numbers those small number of people are seeking to impact via expansion of their now even more disproven as ‘doing good’ (ie it’s pretty obvious reading anything with intelligent eyes it will cause harm in at least one of many possible ways) ideological based business
Then it’s hard to see it as anything other than ‘something else’ very very thinly and poorly charading ‘as if’ it is either healthcare or help or good for those targeted by it. And that’s scary if people as bystanders still choose to not open their eyes to that.
Utsikt
Senior Member (Voting Rights)
21 is unblinded trial:Studies on patients in the longest-running clinic have shown that the treatment is effective and well tolerated by patients [21, 22].
Cognitive–behavioural group treatment for a range of functionalsomatic syndromes: Randomised trial | The British Journal of Psychiatry | Cambridge Core
Cognitive–behavioural group treatment for a range of functionalsomatic syndromes: Randomised trial - Volume 200 Issue 6
Primary outcome:
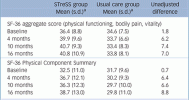
Fully compatible with bias alone.
22 is this drug trial of Imipramine, a tricyclic antidepressant:
They used some weird outcome that will always favour the arm with bias, because it looks at in-group changes:
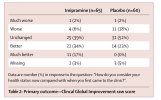
This commentary points out significant issued with blinding, maning the use of subjective outcomes problematic:
If this is all they’ve got to back up their approach, Denmark has some explaining to do..
Re- education I think is the term used instead of coercive psychology/brainwashing/straight coercion (behave right or we will keep you locked up until you will say you have something you don’t, own it, and then have that over your head lifelong )Outpatient treatment clinics
Inpatient services
None of this I feel now is even near the territory of ‘health’ or any of the allieds to it or anything that can use that term within it.
The only way it is related is that it’s targeting the people it wants to earmark (by demographic and face fits I suspect) at the point of getting unwell with something else and fishing them in by pretending they still are safe accessing healthcare like others when ill with something (though it sounds like they will never be tested or diagnosed with what they do have just labelled with something that black marks them from that system)
And in using , errantly, powers not given to them by recalibrating what and who can be accused of mental health to have imposition held over them.
To do things that aren’t health or science for good but behavioural impositions with no therapeutic value and probable harm to the person. Long term.
To me this reads like a plan to ‘take care of/deal with’ and then being nice and ambiguous to allow who gets chosen to be unclear and potentially include anyone but particularly targeting certain types and ideas. It’s really insidious and dangerous.
The new undesirables and place to deal with them defined based on nothing specific enough that anyone can prove it’s not or they are not affecting access points to all parts of everyday life.
To me all I can think of is it being a version of going back to the days where women knew if tgeir husband got fed up they could be taken to be locked in the asylum for the rest of their life. Except now we’ve ‘benevolent’ niche of medics trying to create a system where other medics are conned into doing that
I can’t work out whether it is just for earning money, status etc or now it’s bigger than that and driven by a real problem with certain demographics particularly where they won’t behave as they like etc. Or expect the same rights to healthcare as eg said medics would get if they got ill eg with cancer or Parkinson’s (I doubt they’d expect to be called FND or FMD and anxiety with recommendations not to do tests ever to encourage them).
I do feel like this happens and the only test for it would be that the inventors and instigators should be the first subject to it for x years themselves and what can be rolled out is only what they will themselves ensure - if they want to b spend years being reeducated at harm and have a label ensuring they will never be treated for any real medical issue that they ever get in their lifetime that will never be removed for a few decades to prove it’s not just harm that still doesn’t prove much but at least I’d know if they didn’t have a sneaky get out that they were actually that deluded they’d sign themselves up and not the alternative where they know underneath it all that what they are suggesting is really not good and hence only for others by their selection. Etc
I see no mention of efficacy.The Danish national strategy for FSD has been successfully implemented and integrated into the Danish health care system, achieving organizational integration and high levels of patient and physician satisfaction. The program provides a comprehensive, accessible, and evidence-based framework for managing FSD through a stepped-care approach and may serve as an inspiration for implementation in other countries.
All the form of science and none of the content. This is just marketing. Straight propaganda. Justifying an already failed system installed way ahead of the evidence.
That is exactly what it is happening. All because a few gargantuan egos can't admit they and the lurid fairy-tales in their heads are wrong.Sounds like a manifesto for forcing a dystopia where huge amounts of patients with real illnesses get systemically destroyed /taken apart /removed from rights
It is a blatant social control mechanism, that lacks any technical or moral legitimacy.
And the more wrong they are, and the more status and power and protection they are given, the more ruthless and cruel will become become their resistance to being exposed and held to account for it all.
Joan Crawford
Senior Member (Voting Rights)
21 is unblinded trial:
Cognitive–behavioural group treatment for a range of functionalsomatic syndromes: Randomised trial | The British Journal of Psychiatry | Cambridge Core
Cognitive–behavioural group treatment for a range of functionalsomatic syndromes: Randomised trial - Volume 200 Issue 6www.cambridge.org
Primary outcome:
View attachment 31909
Fully compatible with bias alone.
22 is this drug trial of Imipramine, a tricyclic antidepressant:
They used some weird outcome that will always favour the arm with bias, because it looks at in-group changes:
View attachment 31910
This commentary points out significant issued with blinding, maning the use of subjective outcomes problematic:
If this is all they’ve got to back up their approach, Denmark has some explaining to do..
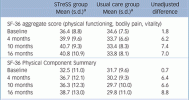
Anyone who with a straight face thinks these outcome functioning scores are anything other that very poorly functioning people post 'intervention' is deluding themselves.
From recall so may not be accurate: Population scores for Physical functioning in mid adulthood is in the top 80s. Scores in the 30s are incredibly low.
Baffling how this low quality churn gets through peer review.
Last edited:
Wait, so they renamed them, then renamed them, then renamed them again to avoid controversy and confusion. Even as they admit to play to the controversy over psychiatric attribution, which is systematically happening, with nonsensical explanations.Over the past decades, numerous specialty-specific functional somatic syndromes (FSS) such as irritable bowel syndrome, fibromyalgia, chronic fatigue syndrome, and most recently long-COVID have been introduced, and new syndromes continue to emerge. Studies consistently demonstrate a huge overlap between these syndromes [9,10]. The unifying evidence-based diagnosis bodily distress syndrome (BDS) was introduced in 2007 [2] This diagnosis has been rigorously validated across clinical settings [3], and it has been shown to be able to replace the functional syndrome diagnoses [9, 24]. In 2019, the BDS diagnosis was included in the Danish ICD-10 as a neutral R-diagnosis, thus avoiding controversies about psychiatric versus non-psychiatric classification [1,11]. The terminology was, however, changed to FSD to avoid confusion with the new but different ICD-11 diagnosis termed bodily distress disorder [1].
Damn it's wild what people will justify when they can just do whatever they want but none of it is real.
Last edited:
That's the perverse beauty of being in total control: no one has to explain anything here, they just do it and no one cares either way.If this is all they’ve got to back up their approach, Denmark has some explaining to do..
Yes it’s pure power.Wait, so they renamed them, then renamed them, then renamed them again to avoid controversy and confusion. Even as they admit to play to the controversy over psychiatric attribution, which is systematically happening, with nonsensical explanations.
Damn it's wild what people will justify when they can just do whatever they want but none of it is real.
So they got away with putting a version (bdd) of what is somatic symptom disorder in the us into their ic10, and then changed it once it was in for the ic11.
And as that is a terrifying in my opinion shouldn’t exist abyss of a non-diagnosis to be allowed to exist - basically even theoretically someone with cancer wouldn’t be excluded from ending up under it even if their physical symptoms were caused by cancer as its main change was removing exclusions where it was explained by a diagnosed medical condition (which I think should be in human rights law, as it’s basically logic) as long as the person in power could claim ‘B list symptoms’ which you know could be them claiming anxiety even tho someone could actually be pretty cool for a person with cancer and all the financial employment etc fall out from it.
So it feels like there is something akin to the sensitivity/specificity issue you get talked about for biomarkers going on here too. No one even talks about false positives being possible?
It’s basically giving power to people who claim it is an ‘R neutral diagnosis’ whatever that is ? Does it mean non psych medics can impose it on a record too as well as psych? And that no one is now empowered to remove or disputes it (would have in the past eg with where it should be if someone called conversion disorder for shakes from one dr then got a scan showing Parkinson’s would that suggested of it having been conversion disorder removed) ?
And by R neutral do they mean it doesn’t come with powers that take away right to choose, second opinion and remove as a diagnosis? I doubt it. Does it possibly somehow despite being neutral come with all the powers of enforcing and compelling said ‘treatments’ using mental health acts and capacity claims despite claiming not to be psychiatric? I’d bet so.
And particularly if you keep getting ill from such mistreatment and are surrounded by those claiming mind they’ll eventually find a way ‘fir your own good’ because those don’t require the treatment to either work or be demonstrated to be the right thing/diagnosis just the person seeking to impress others that they think ‘that’s what’s best’ with no follow up to see if long-term they weren’t made worse by it or died because investigation was refused and a missed diagnosis killed them or meant delayed treatment etc.
Because its premise is once you’ve been labelled ‘even your illnesses were caused by your mind’ … and once it’s under that then noone need provide proof of mechanism. And any future symptom and new illness they assume is the patient failing to fix their faulty thinking that caused the rest.
You can only half escape the power (be released temporarily but never access real medical care as the label overshadows future diagnoses) eg to get discharged by not denying the diagnosis (even if you don’t believe it) and then performing that you are more well by pretending to behave right and saying you are cured, to get out of a facility that will be making you more unwell by the day, it’s pure coercion of any poor sod of the population unlucky enough to be near the wrong people using it. then there’s the vicious cycle that such coerced performance just to get out from under something harming gets counted as ‘recovery claims’ as if it works in a good way. So the emperors new clothes goes on.
Once you’ve got the label good luck with complaining about anything. If it doesn’t work it’s you being mad if it’s abuse it’s you being mad and an unreliable witness if you die it’s sad but they say they can only do so much when someone ‘doesn’t want to get better’ because of their mind.
Yet ignorant bystanders just fall for the ‘it’s only for special people that need to worry about it’ tripe and are told to assume they don’t know the full story if that person seems very sane and normal just biomedically ill and talking sense.
Last edited:
