jnmaciuch
Senior Member (Voting Rights)
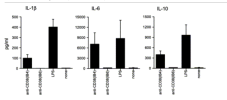
CD38 ligation plays a direct role in the induction of IL-1β, IL-6, and IL-10 secretion in resting human monocytes
Abstract
CD38 signaling, either induced by ligation with specific agonistic monoclonal antibody (mAb) or after interaction with CD31, its cognate counter-receptor, is involved in release of IL-1β, IL-6, and IL-10 cytokines in resting human monocytes. CD38 ligation by the F(ab′)2 IB4 mAb did not induce signals relevant for cytokine secretion and the block of the Fcγ receptor I (FcγRI) by anti-CD64 or FcγRII by anti-CD32 mAb did not inhibit CD38-mediated IL-1β release. Dimerization or multimerization of the CD38 molecule by: (i) cross-linking of the receptor ligated by F(ab′)2 or by (ii) increasing CD38 expression by treating monocytes with IFNγ were able to restore the truncated CD38-mediated signals involved in cytokine secretion. These data indicate that CD38 receptor-mediated signals operate directly suggesting a Fcγ receptorial surface molecule independent activation pathway. The key element for the receptor mediated signaling is represented by surface density of CD38 on resting monocytes.
Web | DOI | Cellular Immunology
Lande, Roberto; Urbani, Francesca; Di Carlo, Beatrice; Sconocchia, Giuseppe; Deaglio, Silvia; Funaro, Ada; Malavasi, Fabio; Ausiello, Clara M.
Abstract
CD38 signaling, either induced by ligation with specific agonistic monoclonal antibody (mAb) or after interaction with CD31, its cognate counter-receptor, is involved in release of IL-1β, IL-6, and IL-10 cytokines in resting human monocytes. CD38 ligation by the F(ab′)2 IB4 mAb did not induce signals relevant for cytokine secretion and the block of the Fcγ receptor I (FcγRI) by anti-CD64 or FcγRII by anti-CD32 mAb did not inhibit CD38-mediated IL-1β release. Dimerization or multimerization of the CD38 molecule by: (i) cross-linking of the receptor ligated by F(ab′)2 or by (ii) increasing CD38 expression by treating monocytes with IFNγ were able to restore the truncated CD38-mediated signals involved in cytokine secretion. These data indicate that CD38 receptor-mediated signals operate directly suggesting a Fcγ receptorial surface molecule independent activation pathway. The key element for the receptor mediated signaling is represented by surface density of CD38 on resting monocytes.
Web | DOI | Cellular Immunology
Last edited: